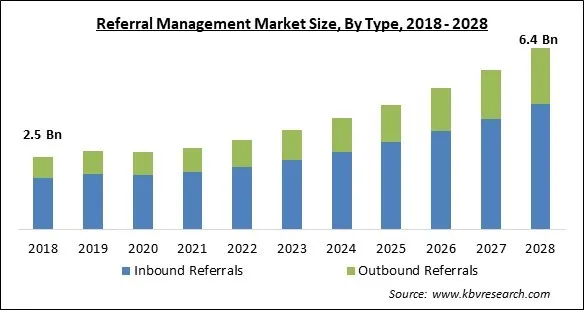
The Global Referral Management Market size is expected to reach $6.4 billion by 2028, rising at a market growth of 12.7% CAGR during the forecast period.
Referral management is defined as the management of the procedure by which patients move on to the subsequent phase of their care. This adjustment typically takes place when a patient's condition is at its most vulnerable during an increase in treatment or a change in diagnosis. Referral management typically occurs when a primary care physician refers a patient to a specialist, but it can also take place when a patient is transferred from an inpatient facility or emergency room to another specialist or to a provider.
Enhancing and streamlining communication between primary care physicians, specialists, and other healthcare providers is the main goal of the referral management system. Modern healthcare is geared toward maximizing quality and effectiveness while lowering costs. The entire sector is adjusting to the use of technology to streamline administrative processes. The widespread use of electronic medical record software in hospitals and clinics across the country is proof of this.
A step in the right direction has been made with the transition to a more standardized and organized approach to documenting and caregiving. When these highly acclaimed Electronic medical records (EMRs) are accompanied by a patient's health insurance or any other health care that they might have, they provide all necessary information to the doctor. This enables both, the doctor and the patient to choose the best method to cure the problem. EMRs are often found by organizations to be insufficient for managing and monitoring referrals.
When health systems have referring clinicians who utilize multiple EMRs or are coordinating treatment between employed and independent doctors, referral management becomes especially crucial. It also finds usage in the management of one or more value-based plans by health systems. Referral management systems aim to enhance patient accessibility and appointment scheduling functionality as well. Their widespread use is also valued when health systems build and oversee a high-performance network of experts.
The healthcare systems around the world were not able to handle the COVID-19 crisis. As it was an unforeseen, significant health issue that demanded an immediate mobilization of resources and impacted the entire population. The pandemic contrasted sharply with the path that healthcare systems, especially in affluent nations, have been heading in recent years. Rather than having any positive or negative effects, the pandemic facilitated the downfall of the overall healthcare structure in many countries. The inconsistent health care industry realized the importance of proper patient management during the pandemic.
A comprehensive range of public health services, such as medical, dental, behavioral, and other patient care, are offered by government organizations, including those at the federal, state, county, and many municipalities. These services, which can be significant in large urban areas, are operable in public hospitals, clinics, nursing homes, and treatment facilities in addition to offering health insurance. Usually, smaller public health agencies provide fewer services. Regardless of the size and scope of the business, the governments recognize that the services provided are crucial for the well-being of the patient population they serve.
Referral programs become harder for people to refer to someone else if they come with too many steps. The manual method often has lower success rates as well. The introduction of automation, along with other significant technology inclusion, has made referral a one-step process. The other benefit of automation and technological inclusion in referral management includes time utilization, improved patient access, and quality patient time. Improvements in patient access are another advantage of the referral management system. The technology allows patients to make appointments based on their availability and the specialist's availability.
Gaps in program execution are caused by the lack of sufficient IT professionals in the healthcare sector, particularly among healthcare providers. Utilizing technology-integrated solutions effectively necessitates a solid IT infrastructure and assistance both inside the firm and from the solution vendor. In healthcare businesses, there is a constant need for technical assistance to maintain the server and network. A very specific skill set is needed to merge knowledge of internal medicine, healthcare insurance, business, and information technology.
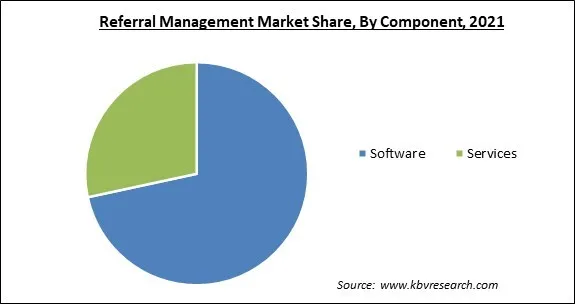
Based on the component, the referral management market is bifurcated into software and services. The services segment procured a significant revenue share in the referral management market in 2021. The referral management services are getting better with each passing day. So patients, who do not have referral management from their providers, choose one themselves. The referral management services usually have third-party characteristics.
On the basis of type, the referral management market is segmented into inbound referrals and outbound referrals. The inbound type segment dominated the referral management market with the largest revenue share in 2021. The huge amount of inbound referrals that hospitals and specialty centers receive from various channels is what is causing this category to rise. A patient does not have to establish credibility and validate assumptions when using an inbound referral.
Based on mode of delivery, the referral management market is categorized into cloud-based and on-premise. The cloud-based segment dominated the referral management market with the highest revenue share in 2021. Due to the advantages of cloud-based solutions, such as on-demand self-serving analytics, no upfront capital investment for hardware, and extreme capacity flexibility, among others, their strong growth rate in this market can be credited.
On the basis of end user, the referral management market is divided into providers, payers, and other end users. The payer segment procured a substantial revenue share in the referral management market in 2021. Healthcare payers who are in charge of managing the treatment of their insured population want to see that patients receive the recommended care as soon as possible.
| Report Attribute | Details |
|---|---|
| Market size value in 2021 | USD 2.9 Billion |
| Market size forecast in 2028 | USD 6.4 Billion |
| Base Year | 2021 |
| Historical Period | 2018 to 2020 |
| Forecast Period | 2022 to 2028 |
| Revenue Growth Rate | CAGR of 12.7% from 2022 to 2028 |
| Number of Pages | 224 |
| Number of Tables | 413 |
| Report coverage | Market Trends, Revenue Estimation and Forecast, Segmentation Analysis, Regional and Country Breakdown, Competitive Landscape, Companies Strategic Developments, Company Profiling |
| Segments covered | Type, Component, Mode of Delivery, End User, Region |
| Country scope | US, Canada, Mexico, Germany, UK, France, Russia, Spain, Italy, China, Japan, India, South Korea, Singapore, Malaysia, Brazil, Argentina, UAE, Saudi Arabia, South Africa, Nigeria |
| Growth Drivers |
|
| Restraints |
|
Based on region, the referral management market is analyzed across North America, Europe, Asia Pacific, and LAMEA. The North American region dominated the referral management market with the maximum revenue share in 2021. Most health insurance providers as well as healthcare providers have already accepted referral management as an integral part of healthcare. The way these work efficiently to save time for patients and providers has also gained support for the referral management systems.
Free Valuable Insights: Global Referral Management Market size to reach USD 6.4 Billion by 2028
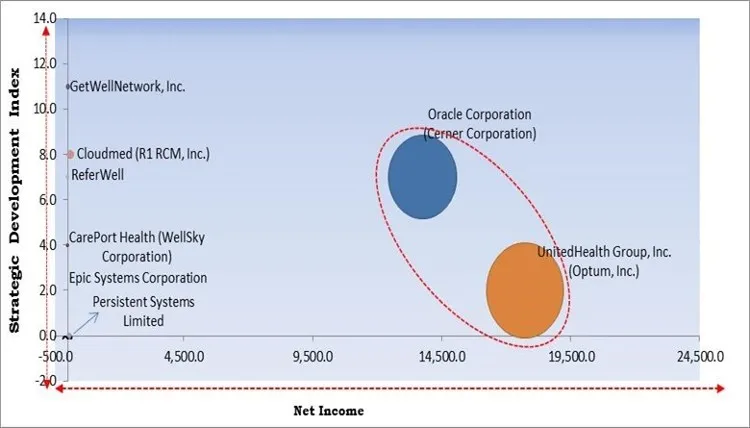
The major strategies followed by the market participants are Partnerships. Based on the Analysis presented in the Cardinal matrix; Oracle Corporation (Cerner Corporation) and UnitedHealth Group, Inc. (Optum, Inc.) are the forerunners in the Referral Management Market. Companies such as GetWellNetwork, Inc., Cloudmed (R1 RCM, Inc.), CarePort Health (WellSky Corporation) are some of the key innovators in Referral Management Market.
The market research report covers the analysis of key stake holders of the market. Key companies profiled in the report include GetWellNetwork, Inc., Epic Systems Corporation, Oracle Corporation (Cerner Corporation), CarePort Health (WellSky Corporation), eHealth Technologies, Inc., UnitedHealth Group, Inc. (Optum, Inc.), Persistent Systems Limited, Cloudmed (R1 RCM, Inc.), EcoSoft Health, and ReferWell.
By Type
By Component
By Mode of Delivery
By End User
By Geography
The global Referral Management Market size is expected to reach $6.4 billion by 2028.
Provision Of Inclusion Of Referral Management In Healthcare By Government are driving the market in coming years, however, Lack Of Skilled Healthcare Information Management Professionals restraints the growth of the market.
GetWellNetwork, Inc., Epic Systems Corporation, Oracle Corporation (Cerner Corporation), CarePort Health (WellSky Corporation), eHealth Technologies, Inc., UnitedHealth Group, Inc. (Optum, Inc.), Persistent Systems Limited, Cloudmed (R1 RCM, Inc.), EcoSoft Health, and ReferWell.
The Software segment acquired maximum revenue share in the Global Referral Management Market by Component in 2021 thereby, achieving a market value of $4.4 billion by 2028.
The Providers segment is leading the Global Referral Management Market by End User in 2021 thereby, achieving a market value of $3 billion by 2028.
The North America market dominated the Global Referral Management Market by Region in 2021, and would continue to be a dominant market till 2028; thereby, achieving a market value of $2.4 billion by 2028.
Our team of dedicated experts can provide you with attractive expansion opportunities for your business.

